What is Pre-implantation Genetic Testing for Aneuploidies (PGT-A)?
At Sunfert, we offer Pre-implantation Genetic Testing for Aneuploidies (PGT-A) as a genetic screening tool to examine embryos created through IVF before they are transferred to the uterus.
PGT-A helps us identify whether an embryo has the correct number of chromosomes. Chromosomes carry genetic information, and a healthy embryo typically contains 46 chromosomes arranged in 23 pairs.
How are Embryos Screened using Advanced Genetic Technology?
To perform PGT-A accurately, we use a technology called Next-Generation Sequencing (NGS) at Sunfert. This is a top-notch advanced genetic testing technology in the industry that allows us to examine the DNA of an embryo in detail, helping us determine whether it has the correct number of chromosomes.
During the PGT-A process, a few cells are carefully taken from the embryo and analysed using NGS. This technology can screen all 23 pairs of chromosomes at once with high precision, allowing us to identify embryos that are chromosomally normal as well as those with chromosomal abnormalities. By selecting embryos with the correct chromosomal count, PGT-A helps improve the chances of successful implantation, supports a healthier pregnancy, and reduces the risk of miscarriage for patients undergoing IVF.
What are Chromosomal Abnormalities?
A normal embryo has 23 pairs of chromosomes. Chromosomal abnormalities occur when there is an extra chromosome, a missing chromosome, or a structural imbalance in the embryo. These abnormalities may increase the risk of:
- Implantation failure
- Miscarriage
- Genetic disorders
By screening embryos before transfer, we aim to select embryos with the correct chromosomal count to improve the chance of establishing a healthy pregnancy.
Examples of Chromosomal Abnormalities
Some disorders that arise from chromosomal abnormalities include:
- Down’s Syndrome (Trisomy 21): caused by extra copy of chromosome 21
- Edwards’ Syndrome (Trisomy 18): caused by extra copy of chromosome 18
- Patau’s Syndrome (Trisomy 13): caused by extra copy of chromosome 13
- Turner Syndrome (Monosomy X): caused by a missing copy of chromosome X in female embryos
- Other numerical chromosomal abnormalities (aneuploidies) may lead to implantation failure or miscarriage
When combining IVF treatment with PGT-A, we can reduce the risk of transferring embryos with detectable chromosomal abnormalities.
Who Should Consider PGT-A?
We generally recommend PGT-A for individuals or couples who:
- are at an advanced maternal age
- have had recurrent miscarriages
- have experienced recurrent implantation failure
- have previously had a pregnancy affected by chromosomal abnormalities
- produce multiple embryos and want to prioritise chromosomally normal embryos
- wish to reduce the risk of transferring embryos affected by disorders such as Down’s Syndrome
At Sunfert, we assess each case individually to determine whether PGT-A is clinically appropriate for our patients’ fertility journey.
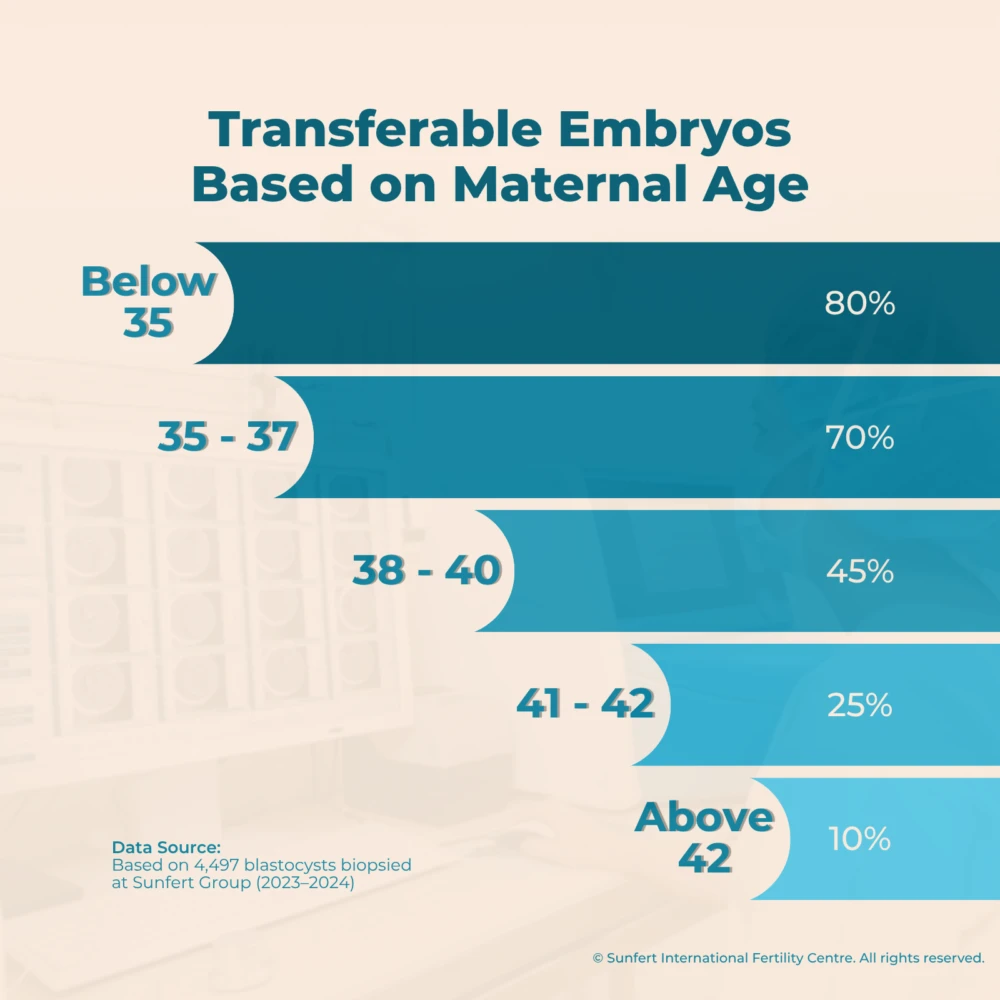
Our data and research at Sunfert shows that PGT-A benefits women of all age groups, especially those with advanced maternal age. As age increases, the number of transferable embryos decreases, and PGT-A can help identify the healthiest embryos for a higher chance of success.
Who Can Benefit from PGT-A?
PGT-A can benefit patients who want greater confidence in embryo selection before transfer.
We often see positive value for those who:
- are planning pregnancy at a later reproductive age
- want to minimise miscarriage risk linked to chromosomal abnormalities
- aim to increase the IVF treatment success rate with a more targeted, evidence-based embryo transfer plan.
For many patients, it provides reassurance by giving us additional genetic insight into the quality of their embryos.
Click here to learn more about Sunfert Success Rate?
How is PGT-A Performed at Sunfert?
Step 1: IVF Treatment & Embryo Development
We stimulate the ovaries, retrieve the eggs, and fertilise them in our laboratory through IVF/ICSI.
The embryos are cultured until they reach the blastocyst stage (Day 5 or Day 6).
Step 2: Embryo Biopsy
Performed by our highly-trained embryologists or genetic scientists, a tiny cluster of cells is collected from the outer layer of the blastocyst (trophectoderm biopsy).
Step 3: Pre-implantation Genetic Testing for Aneuploidies
The biopsied cells undergo chromosomal testing using advanced genetic technology to determine if the embryo has the correct number of chromosomes.
The results are generated and shared with our patients and fertility specialists within 2 to 3 weeks.
Step 4: Embryo Selection and Transfer
Embryos identified as chromosomally normal (euploid) are prioritised for transfer in a subsequent cycle to improve the likelihood of a healthy pregnancy.
Mosaic embryos, which contain a mix of normal and abnormal cells, may be considered for transfer in selected cases following careful clinical evaluation and counselling.
Take the Next Step with Our Fertility Specialists
If you are facing fertility challenges, start with a consultation at Sunfert. We will guide you through your fertility journey with expertise and compassionate care.
Make an appointment with our Fertility Specialist today and take the next step toward your parenthood goals.
Frequently Asked Questions About PGT-A
Question #1: What is the main purpose of PGT-A?
- PGT-A screens embryos for chromosomal abnormalities before transfer, helping select those with the best chance of implantation and a healthy pregnancy.
Question #2: Is PGT-A recommended for everyone undergoing IVF?
- PGT-A is typically recommended for selected patients based on factors such as age, medical history, recurrent miscarriage, repeated IVF failure, or with known chromosomal structural abnormalities, although some patients may choose it to support better-informed embryo selection.
Question #3: Is embryo biopsy safe?
- Embryo biopsy requires a tremendous amount of training and years of experience, supported by a well-established procedure.
- At Sunfert, we ensure that all our embryologists and genetic scientists are well trained and strictly follow established protocols. Hence, we are confident that the biopsy procedures performed at Sunfert are safe for patients’ embryos.
Question #4: How long does the PGT-A testing result take?
- At Sunfert, our patients are able to receive their results within 2 to 3 weeks after the biopsy process.
Question #5: Can PGT-A detect genetic diseases?
- No. PGT-A screens for chromosomal abnormalities (aneuploidies) but does not detect single-gene disorders unless combined with additional genetic testing.
- Patients who are concerned about passing on inherited genetic disorders to their next generation are advised to undergo Pre-implantation Genetic Testing for Monogenic disorders (PGT-M).

