Why Personalised Fertility Treatment Matters?
At Sunfert International Fertility Centre, we believe every patient deserves personalised fertility care and treatment because no two fertility journeys are the same.
Hence, our fertility specialists will:
- assess your age, ovarian reserve, and medical history
- customise treatment plan based on your body’s response
- prioritise minimal discomfort and shorter treatment duration
- aim to maximise your chances of success
What IVF Stimulation Protocols Are Available at Sunfert?
At Sunfert International Fertility Centre, we offer a range of clinically proven IVF stimulation protocols. Each protocol is carefully selected based on your individual fertility condition to optimise outcomes while ensuring your safety and comfort throughout the treatment journey.
The available stimulation protocols include:
- Long Down Regulation Protocol (LDR)
- Short GnRH Antagonist Protocol
- Microflare Protocol
- Natural Cycle IVF
Short GnRH Antagonist Protocol
Who Is This Protocol Suitable For?
- Women with PCOS
- Patients at risk of OHSS
- Those who prefer a shorter and more patient-friendly protocol
How Does This Protocol Work?
- May begin with oral contraceptive pills (OCPs)
- FSH injections start on Day 2 or Day 3 of the cycle
- A GnRH antagonist (e.g. Cetrotide or Orgalutran) is introduced mid-cycle
- This prevents premature release of eggs
What Is the Treatment Timeline?
- Total duration: Around 10 to 12 days
- Monitoring scan typically performed on Day 5
- Daily injections continue until egg maturation
Short GnRH Antagonist Protocol Treatment Timeline
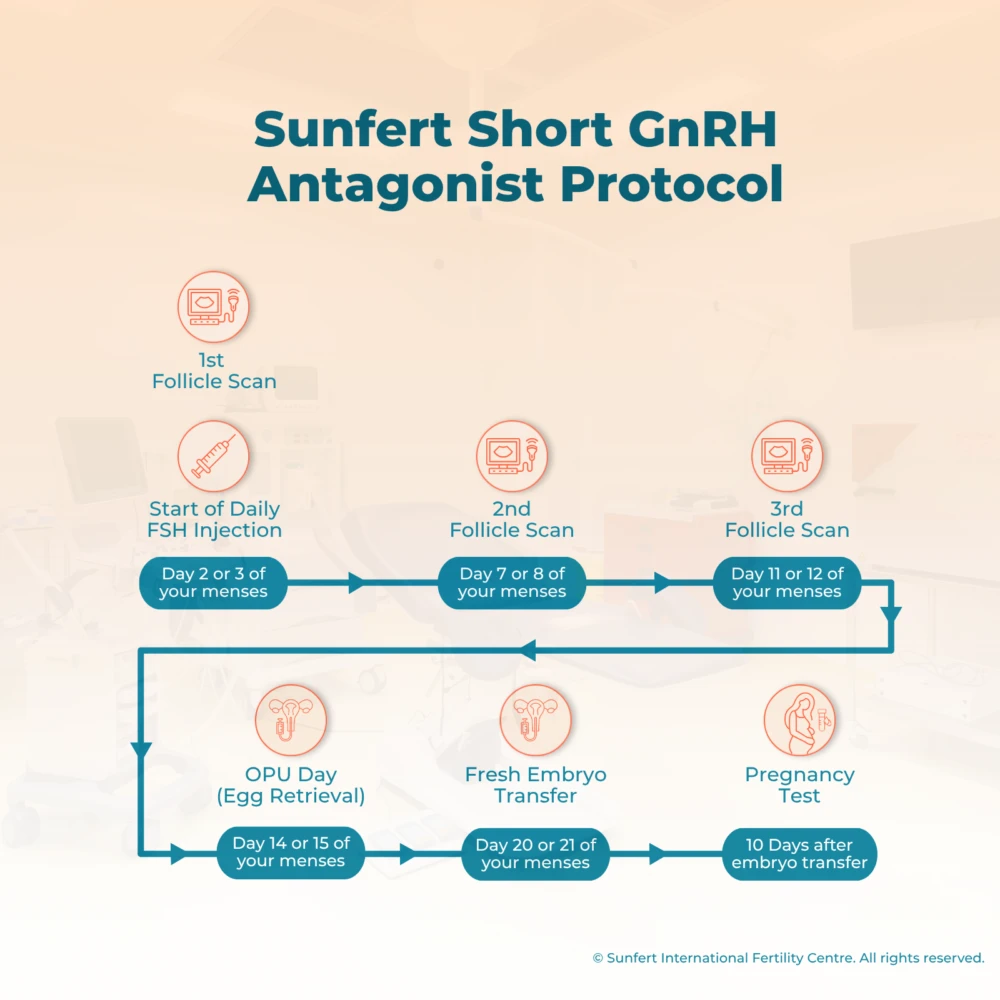
Long Down Regulation Protocol (LDR)
Who Is This Protocol Suitable For?
- Women with endometriosis (including undiagnosed cases)
- Patients who require stronger hormonal control
- Those seeking a well-established protocol with consistent outcomes
How Does This Protocol Work?
- Begins around Day 21 of your menstrual cycle
- A scan confirms ovulation before starting treatment
- Daily Buserelin (Suprefact) injections suppress ovarian activity
- Once suppression is achieved, ovarian stimulation begins with FSH injections
- A GnRH antagonist may be added mid-cycle to prevent premature ovulation
What Is the Treatment Timeline?
- Total duration: Approximately 4 weeks or longer
- About 2 weeks for down regulation
- Followed by 10 to 12 days of ovarian stimulation
- Multiple scans are performed to monitor progress
Long Down Regulation Protocol Treatment Timeline
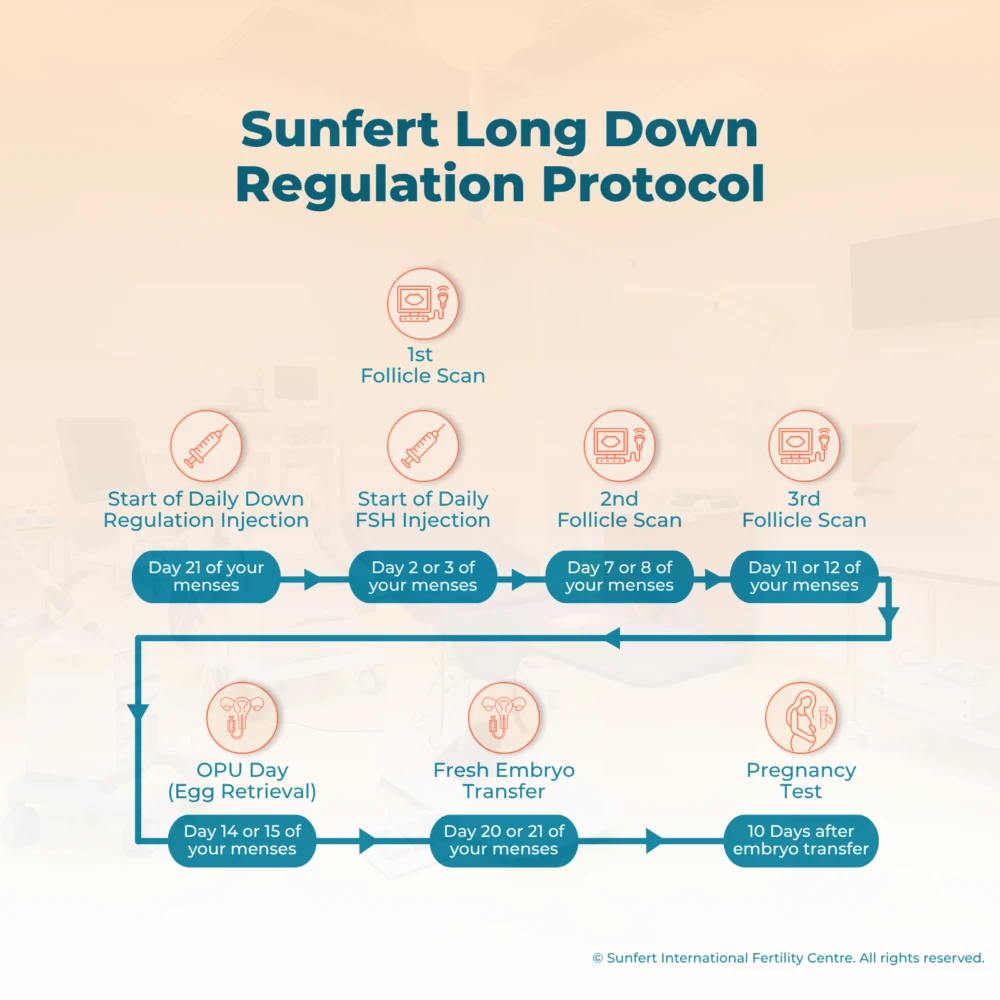
Microflare Protocol
Who Is This Protocol Suitable For?
- Women above 35 years old
- Patients with low ovarian reserve
- Those who had poor response in previous IVF cycles
How Does This Protocol Work?
- Pre-treatment with oral contraceptive pills
- Low-dose Buserelin starts on Day 2 of menstruation to stimulate ovarian response
- FSH injections begin from Day 3 to support follicle development
What Is the Treatment Timeline?
- Total duration: Approximately 10 to 12 days
- Focused stimulation phase to maximise egg production
Microflare Protocol Treatment Timeline
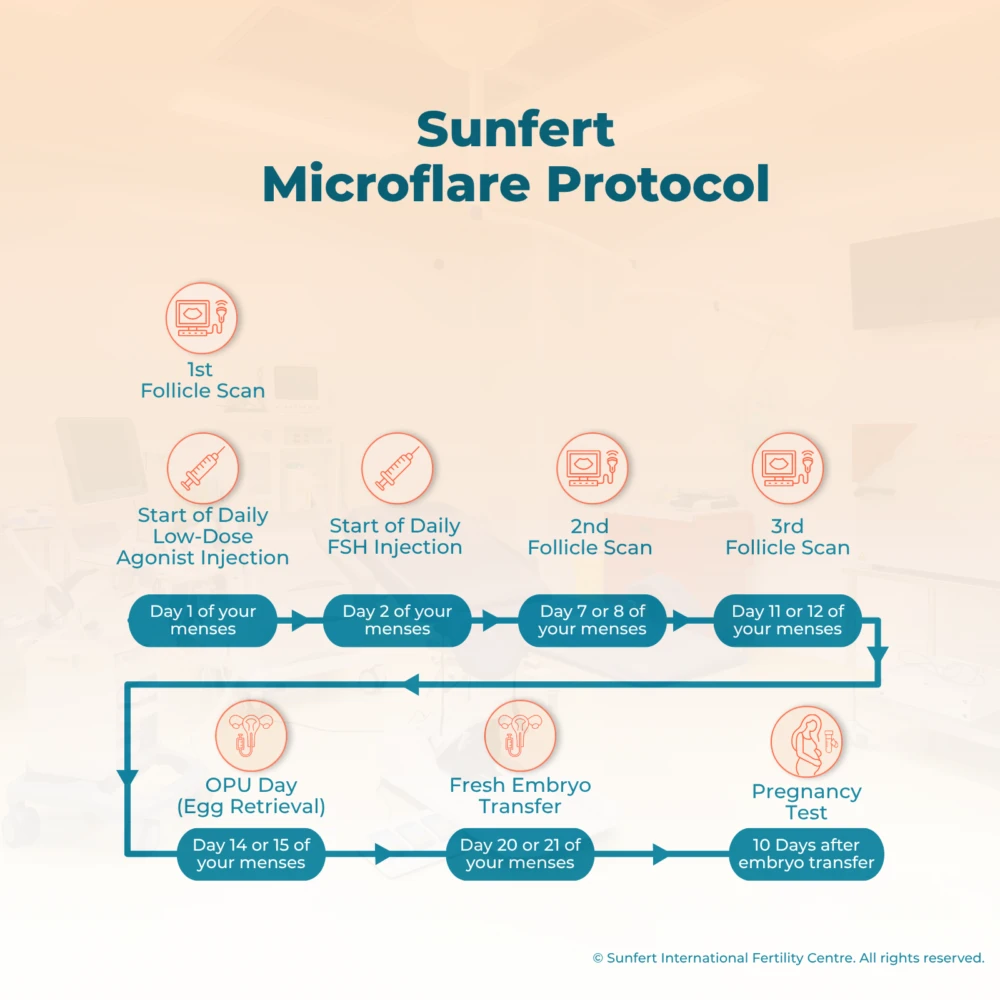
Natural Cycle IVF
Who Is This Protocol Suitable For?
- Women with regular menstrual cycles
- Patients with low ovarian reserve
- Those who prefer minimal medication or a more natural approach
How Does This Protocol Work?
- Minimal or no hormonal stimulation is used
- The body naturally produces one or two eggs
- Eggs are retrieved and fertilised during the IVF process
What Is the Treatment Timeline?
- Shorter and simpler cycle compared to stimulated IVF
- Typically requires about 3 clinic visits for monitoring
- Minimal injections or medications involved
Take the Next Step with Our Fertility Specialists
If you are facing fertility challenges, start with a consultation with our specialists. We will guide you through your fertility journey with expertise and compassionate care.
Make an appointment with our Fertility Specialist today and take the next step toward your parenthood goals.
-
 Book a consultation
Book a consultationDato' Dr Wong Pak Seng
Founder of Sunfert Group & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Eeson Sinthamoney
Group Medical Director & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Lim Lei Jun
Medical Director (Sunfert Bangsar South) & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Sumithra Devi Valiapan
Consultant Obstetrics, Gynaecology & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Haris Njoo Suharjono
Medical Director (Sunfert Kuching) & Fertility Specialist- Sunfert@Kuching

