What is Reproductive Surgery?
Reproductive surgery for males refers to surgical procedures or microsurgical sperm retrieval techniques designed to retrieve sperm or correct anatomical issues that affect fertility.
At Sunfert, we offer advanced microsurgical and minimally invasive techniques to help men with obstructive or non-obstructive fertility challenges achieve biological parenthood.
These procedures are performed by our experienced fertility specialists using precision technology to maximise the chances of successful sperm retrieval.
Male reproductive surgery is typically recommended when:
- sperm is absent in the ejaculate (Azoospermia)
- there is a blockage preventing sperm release
- previous sperm analysis shows severely low sperm count
- assisted reproductive treatment requires direct sperm retrieval
Notes:
- Azoospermia: A condition where no sperm is found in the semen, leading to male infertility.
- Non-obstructive Azoospermia: A form of azoospermia caused by impaired or absent sperm production in the testes.
- Obstructive Azoospermia: A form of azoospermia caused by a blockage that prevents sperm from being present in the semen despite normal sperm production.
Types of Reproductive Surgery for Males
There are 4 main types of minimally invasive reproductive surgery for males available at Sunfert:
Microsurgical Testicular Sperm Extraction (MESA)
Percutaneous Testicular Sperm Aspiration (PESA)
Testicular Sperm Aspiration (TESA)
Testicular Sperm Extraction (TESE)
What is MESA, PESA, TESA and TESE?
Microsurgical Testicular Sperm Extraction (MESA)
MESA is an advanced surgical procedure where we use an operating microscope to carefully identify and extract sperm directly from the testicular tissue.
This technique allows us to precisely locate tiny areas where sperm production may still be occurring, even in challenging cases.
Percutaneous Testicular Sperm Aspiration (PESA)
PESA is a minimally invasive procedure where we use a fine needle to extract sperm from the epididymis. It is performed under local anaesthesia and does not require open surgery.
Note:
- Local anesthesia is used to temporarily numb a specific area of the skin, underlying tissue, and peripheral nerves to reduce pain during minor procedures.
Testicular Sperm Aspiration (TESA)
TESA involves using a needle to extract sperm directly from the testicle. Unlike open surgical methods, TESA is performed through needle aspiration, making it a straightforward and minimally invasive option.
Testicular Sperm Extraction (TESE)
TESE is a minor surgical procedure where we remove a small biopsy of testicular tissue to extract sperm. The tissue sample is carefully examined in our laboratory to identify viable sperm for fertilisation.
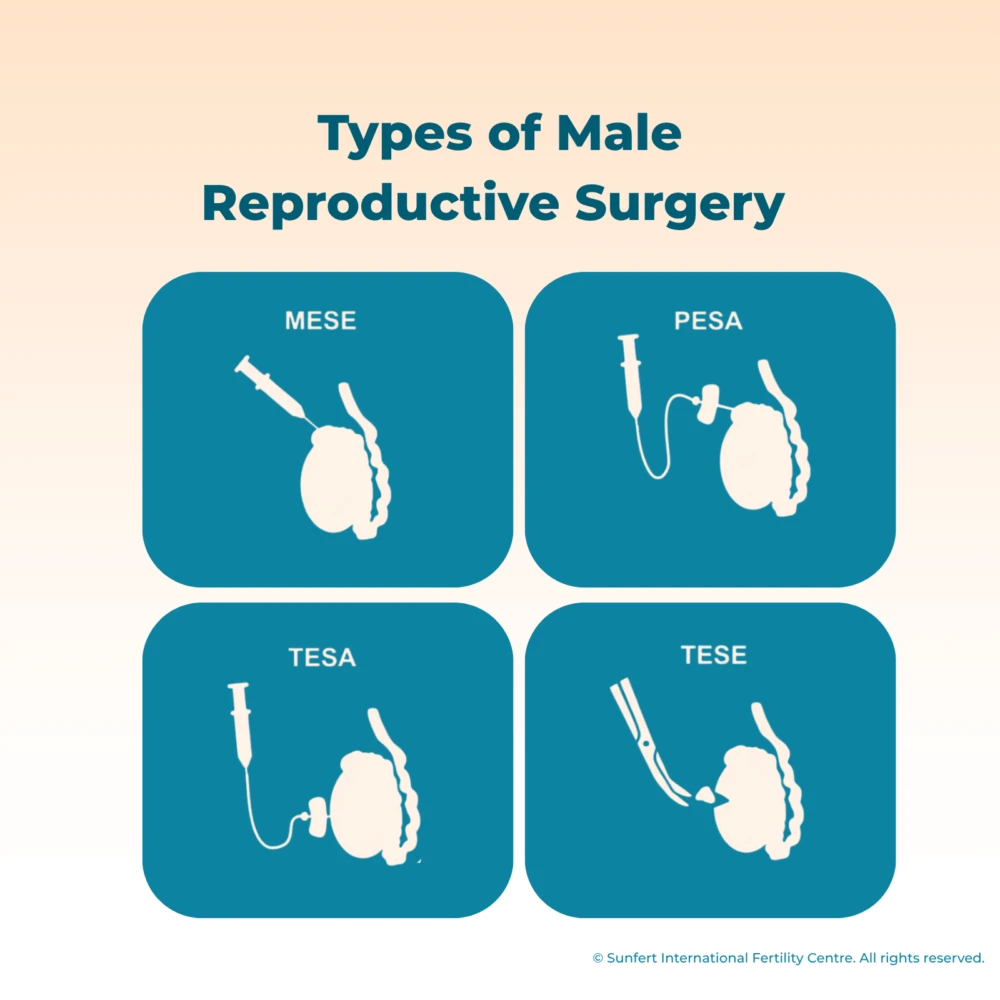
The Difference Between MESA, PESA, TESA and TESE
| Aspect | MESA | PESA | TESA | TESE |
|---|---|---|---|---|
| Procedure Method | Microsurgical retrieval of sperm from the epididymis | Needle aspiration of sperm from the epididymis | Needle aspiration of sperm directly from testicular tissue | Surgical biopsy of testicular tissue to extract sperm |
| When It’s Used | Obstructive azoospermia (blocked sperm ducts) | Obstructive azoospermia | Epididymal sperm unavailable or prior procedure failed | Non-obstructive azoospermia (low or no sperm production) |
| Key Features | High-quality sperm, requires microsurgery | Less invasive, quick outpatient procedure | Simple outpatient procedure, sperm from testicle | Multiple biopsies may be performed for better yield |
| Recovery Time | Minor recovery, small incision | Minimal discomfort, fast recovery | Minor soreness, local anesthesia | Small surgical site, short recovery |
Take the Next Step with Our Fertility Specialists
If you are facing fertility challenges, start with a consultation at Sunfert. We will guide you through your fertility journey with expertise and compassionate care.
Make an appointment with our Fertility Specialist today and take the next step toward your parenthood goals.
-
 Book a consultation
Book a consultationDato' Dr Wong Pak Seng
Founder of Sunfert Group & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Eeson Sinthamoney
Group Medical Director & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Lim Lei Jun
Medical Director (Sunfert Bangsar South) & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Sumithra Devi Valiapan
Consultant Obstetrics, Gynaecology & Fertility Specialist- Sunfert@Bangsar South
-
 Book a consultation
Book a consultationDr Haris Njoo Suharjono
Medical Director (Sunfert Kuching) & Fertility Specialist- Sunfert@Kuching
What is the difference between MESA, PESA, TESA, and TESE?
Microsurgical Testicular Sperm Extraction (MESA): Uses microsurgery to retrieve sperm from the epididymis.
Percutaneous Testicular Sperm Aspiration (PESA): Uses a fine needle to aspirate sperm from the epididymis.
Testicular Sperm Aspiration (TESA): Retrieves sperm directly from the testicle using needle aspiration.
Testicular Sperm Extraction (TESE): Involves taking a small biopsy of testicular tissue to locate sperm.
Each technique is selected based on the underlying cause of infertility.
Is MESA painful and how long is recovery?
Microsurgical Testicular Sperm Extraction (MESA) is performed under anaesthesia to ensure minimal discomfort during the procedure.
Most patients experience mild soreness afterwards, and recovery is usually quick, with many returning to light activities within a few days.
Is PESA safe for treating obstructive azoospermia?
Yes, Percutaneous Testicular Sperm Aspiration (PESA) is a safe and commonly used procedure for obstructive azoospermia.
It is minimally invasive, performed under local anaesthesia, and does not require open surgery.
Recovery is typically fast with minimal discomfort.
Can TESA be repeated if no sperm is found?
Yes, Testicular Sperm Aspiration (TESA) can be repeated if clinically appropriate.
The decision depends on medical evaluation, underlying fertility condition, and previous sperm retrieval outcomes.
Our fertility specialist will advise on timing and suitability for repeat procedures.
When is TESE recommended instead of needle-based sperm retrieval?
Testicular Sperm Extraction (TESE) is usually recommended when needle-based methods like TESA or PESA do not successfully retrieve sperm, or when a larger tissue sample is needed to improve the chances of finding viable sperm, especially in cases of non-obstructive azoospermia.

